

procedures/Hair Transplantation
Hair Transplantation
About
Hair is an important part of our appearance and affects our interactions with others. It can set our mood and confidence level before we even leave the house, and we judge and assess others by theirs, albeit subconsciously.
A healthy, full head of hair reflects youthfulness, attractiveness and success.
Options for hair restoration have been limited and not well understood or trusted- until now.
FUE (Follicular Unit Extraction) using NEOGRAFT is the GOLD standard in Hair Transplantation for Men and Women.
Candidates
Although most individuals will prove to be good candidates, there are some prerequisites.
- No underlying disease causing the hairloss. This should be treated first.
- Enough donor hairs and a healthy recipient site
- Realistic expectations
the procedure
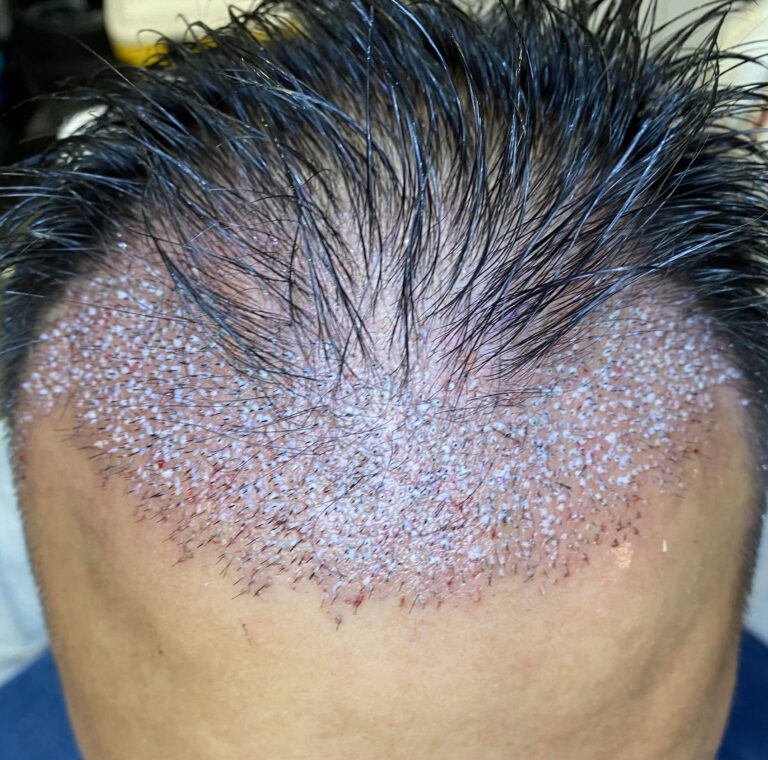
Hair transplantation is performed in our office under local anaesthesia. It is a long procedure, and takes much of the day to perform but we do our best to make sure you are comfortable throughout. You can take breaks as needed, and watch tv, work or nap during much of the procedure.
Components of the procedure are as follows:
- mark up your donor site and new hairline
- make sites for the transplanted hairs
- use Neograft to harvest follicular units from the donor site
- implants the grafts into the recipient area.
FUE Advantage
- Minimal Scarring
- Minimal Pain
- Fast recovery
- Minimal downtime
- Natural Results
Aftercare
We will provide you with a care sheet and take home pack to help look after your new hair post procedure.
We prefer that you have someone pick you up after the procedure, but you can arrange an Uber or Taxi if needed.
Downtime after the procedure is 1-2 weeks, depending on how discreet you wish to be.
You are able to fly the day after the procedure if you come from interstate.
- HAIR FACTS
- HAIR LOSS in MEN
- HAIR LOSS in WOMEN
Hair Facts
The average person has approximately 100 000 hair follicles on their scalp, grouped in follicular units with 1 – 4 hairs.
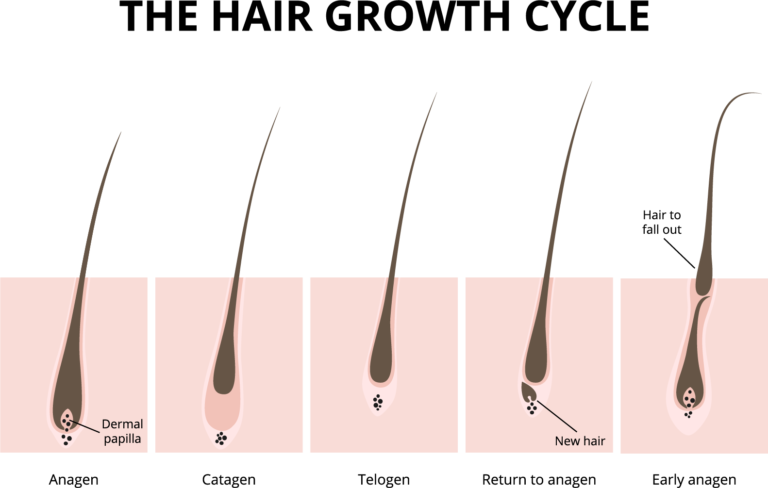
Hair cycles through 3 growth phases, but not all hairs are in the same phase at any one time. Disruption of this cycle will result in hair loss over time.
Anagen = the active growing phase. About 90% of your hairs are in this phase at a given time, usually for a period of 2-6 years.
Catagen = a transition phase between growing and resting, and usually occurs over a period of 2-3 weeks.
Telogen = the resting phase, with no active hair growth. About 10% of your hairs are in this phase at a given time. It is normal to lose up to 100 hairs a day in this phase. Normally these follicles will enter Anagen at the end of this cycle and a new hair will form.
The human eye can’t detect hair loss until at least 50% of the hair in an area has been lost. Thinning is better disguised in those with low colour contrast between their hair and scalp, and more obvious in those with a high contrast, such as black hair and a pale scalp.
Hair Loss in Men
Approximately 50% of men will have noticeable hair loss by the time they are 50. In 95% of these, the cause is Androgenetic Alopecia, more commonly known as Male Pattern Hair loss. This is an inherited condition, but the exact genetics have not yet been determined. We do know that multiple genes are involved, that they may be from either parent and that there is a variable expression of their effect amongst family members, so one brother may be bald and another have a full head of hair.
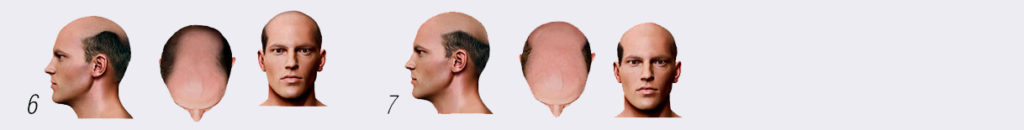
These patterns are classified using the Norwood scale. The patterns are usually progressive, so knowing your family history may be useful in predicting what your eventual hair loss pattern might be. The younger your hair loss starts, the more severe it is likely to be. Stages 1 and 2 are mild to minimal loss, stage 3 is the beginning of clinically significant balding. There is a typical pattern, with progressive loss in both the anterior and vertex area. In some one of these areas is better preserved, theses are noted as types v (vertex) or a (anterior). The most severe types 6 and 7 have the smallest donor site, but the biggest graft demand.
The Norwood Scale




Hair follicles in these individuals are susceptible to the androgen Dihydrotestosterone (DHT) which causes the hairs to become finer (a process called miniaturisation), the growing phase (Anagen) to become shorter and increases the percentage of hairs in the resting phase (Telogen). Medications that decrease the amount of DHT can help to stop the progress of hair loss. Other medications may also help by increasing the percentage of hairs in the growing phase.
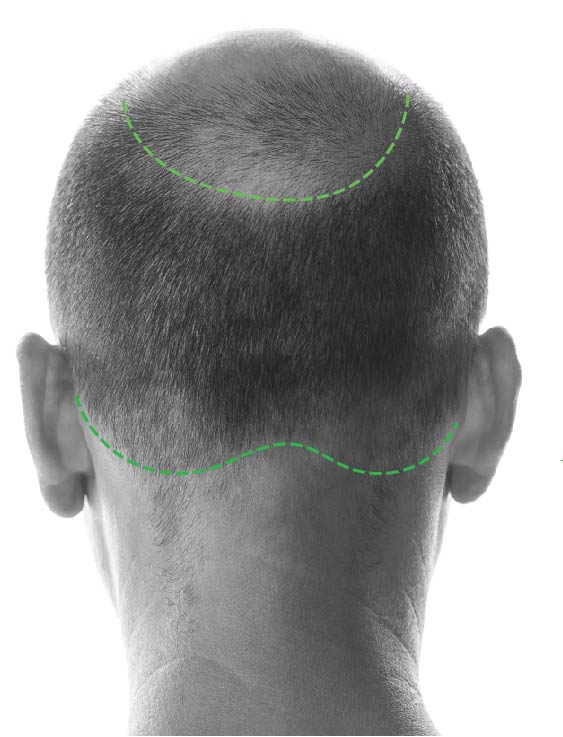
The good news is that there is a stable zone of hairs present at the back and sides of the head, in a U shape. These hairs are not susceptible to DHT and can be used as donors in hair transplantation. Their genetic makeup won’t change when transplanted so they will be permanent.
Hair Loss in Women
Up to 40% of women will experience some form of hair loss by the time they are 50. As with men, the most common cause is Androgenetic Alopecia, aka Female Pattern Hair loss. This is usually later in onset than that in males and has a different distribution. The severity of hair loss is classified using the Ludwig scale.
The Ludwig Scale
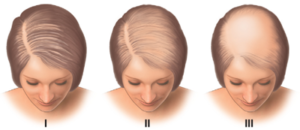
The hair follicles are also susceptible to DHT, but as these levels are much lower in females it may be precipitated by the differing ratio of female hormones as menopause occurs, such that the relative rates of DHT increase. Decreasing DHT production with Finasteride is not effective in the treatment of Female Pattern hair loss and contraindicated because of its potential effect on male embryos in pregnancy. Minoxidil may be useful in some, but is less practical for daily use in women with long hair.
There are several other causes of hair loss in men and women. Although less common, a thorough history and examination will reveal the underlying cause in most.
Hair transplantation is not recommended in patients if the health of their donor hairs or their uptake after transplantation is considered to be poor.
